Body-focused repetitive behavior
In today's world, Body-focused repetitive behavior has become a topic of great importance and relevance. Since its emergence, it has captured the attention of a large number of individuals, either due to its direct impact on society or due to its influence in different areas. Body-focused repetitive behavior has generated controversy, debate and discussion, and its presence continues to generate interest and curiosity in those who wish to further understand its meaning and scope. In this article, we will explore the different aspects related to Body-focused repetitive behavior, from its origin to its evolution in the present, with the aim of providing a comprehensive and comprehensive view on the topic.
| Body-focused repetitive behavior | |
|---|---|
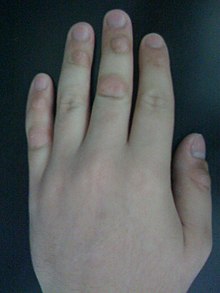 | |
| Dermatillomania (picking of the skin) of the knuckles (via mouth), illustrating disfiguration of the distal and proximal joints of the middle and little fingers |
Body-focused repetitive behavior (BFRB) is an umbrella name for impulse control behaviors involving compulsively damaging one's physical appearance or causing physical injury.
Body-focused repetitive behavior disorders (BFRBDs) in ICD-11 is in development.
BFRB disorders are currently estimated to be under the obsessive-compulsive spectrum. They are also associated with ADHD and anxiety.
Causes
The cause of BFRBs is unknown.[citation needed]
Emotional variables may have a differential impact on the expression of BFRBs.
Research has suggested that the urge to repetitive self-injury is similar to a body-focused repetitive behavior but others have argued that for some the condition is more akin to a substance abuse disorder.[citation needed]
Researchers are investigating a possible genetic component.
Onset
BFRBs most often begin in late childhood or in the early teens.
Diagnosis
Types
- Skin
- Dermatillomania (excoriation disorder), skin picking
- Dermatophagia, skin nibbling
- Mouth
- Morsicatio buccarum, cheek biting
- Morsicatio labiorum, inner lip biting
- Morsicatio linguarum, tongue biting
- Nails
- Onychophagia, nail biting
- Onychotillomania, nail picking
- Nose
- Rhinotillexomania, compulsive nose picking
- Hair
- Trichophagia, hair nibbling
- Trichotemnomania, hair cutting
- Trichotillomania, hair pulling
- Eyes
- Mucus fishing syndrome - compulsion to remove or "fish" strands of mucus from the eye
Treatment
Psychotherapy
Treatment can include behavior modification therapy, medication, and family therapy. The evidence base criteria for BFRBs is strict and methodical. Individual behavioral therapy has been shown as a "probably effective" evidence-based therapy to help with thumb sucking, and possibly nail biting. Cognitive behavioral therapy was cited as experimental evidence based therapy to treat trichotillomania and nail biting; a systematic review found best evidence for habit reversal training and decoupling. Another form of treatment that focuses on mindfulness, stimuli and rewards has proven effective in some people. However, no treatment was deemed well-established to treat any form of BFRBs.
Pharmacotherapy
Excoriation disorder, and trichotillomania have been treated with inositol and N-acetylcysteine.
Prevalence
BFRBs are among the most poorly understood, misdiagnosed, and undertreated groups of disorders. BFRBs may affect at least 1 out of 20 people. These collections of symptoms have been known for a number of years, but only recently have appeared in widespread medical literature. Trichotillomania alone is believed to affect 10 million people in the United States.
See also
- Stereotypic movement disorder
- Rhythmic Movement Disorder
- Body dysmorphic disorder
- Habit reversal training
- Decoupling treatment
References
- ^ a b c "Scientific Advances in Trichotillomania and Related Body-Focused Repetitive Behaviors". National Institute of Mental Health. November 4, 2004. Archived from the original on July 21, 2011.
- ^ a b c d e "AAMFT Consumer Update - Hair Pulling, Skin Picking and Biting: Body-Focused Repetitive Disorders". American Association for Marriage and Family Therapy. Archived from the original on 2009-04-25.
- ^ Grant JE, Stein DJ (2014). "Body-focused repetitive behavior disorders in ICD-11". Revista Brasileira de Psiquiatria. 36 Suppl 1 (suppl 1): 59–64. doi:10.1590/1516-4446-2013-1228. PMID 25388613.
- ^ a b "Trichotillomania (TTM) & Related Body-Focused Repetitive Behaviors (BFRBs)". The Center for Emotional Health of Greater Philadelphia. Archived from the original on 2011-12-29.
- ^ Teng EJ, Woods DW, Marcks BA, Twohig MP (March 2004). "Body-Focused Repetitive Behaviors: The Proximal and Distal Effects of Affective Variables on Behavioral Expression". Journal of Psychopathology and Behavioral Assessment. 26 (1): 55–64. doi:10.1023/B:JOBA.0000007456.24198.e4. S2CID 144926749.
- ^ ABC News 20/20 Hair Pulling, 2006
- ^ a b c d Woods DW, Houghton DC (13 July 2015). "Evidence-Based Psychosocial Treatments for Pediatric Body-Focused Repetitive Behavior Disorders". Journal of Clinical Child and Adolescent Psychology. 45 (3): 227–40. doi:10.1080/15374416.2015.1055860. PMID 26167847.
- ^ Lee MT, Mpavaenda DN, Fineberg NA (2019). "Habit Reversal Therapy in Obsessive Compulsive Related Disorders: A Systematic Review of the Evidence and CONSORT Evaluation of Randomized Controlled Trials". Frontiers in Behavioral Neuroscience. 13: 79. doi:10.3389/fnbeh.2019.00079. PMC 6491945. PMID 31105537.
- ^ Torales J, Barrios I, Villalba J (2017). "Alternative Therapies for Excoriation (Skin Picking) Disorder: A Brief Update". Advances in Mind-Body Medicine. 31 (1): 10–13. PMID 28183072.
- ^ Families & Health Archived March 28, 2009, at the Wayback Machine, American Association for Marriage and Family Therapy
- ^ Diefenbach GJ, Reitman D, Williamson DA (April 2000). "Trichotillomania: a challenge to research and practice". Clinical Psychology Review. 20 (3): 289–309. doi:10.1016/S0272-7358(98)00083-X. PMID 10779896.